Views: 999
Abstract:
The Coronavirus, well known for more than half a century and similar to the Influenza virus, has alarmed most governments. Believing the mode of transmission to be through contact and droplets, the measures taken to deal with the emergency have proved not only inefficient but downright harmful. Thus the way has been cleared for vaccination, superfluous and potentially dangerous like all innovative vaccinations. No action is taken on the true mode of transmission of the virus, which occurs exclusively through aerosols, aggravating the global situation day by day.
Virology originated in 1780 BC (Codex Eschnunna) (1), where a case of rabies was described. In the first century BC Cornelius Aulus Celsus (2) defined the agent of this disease a virus, in 1882 Adolf Mayer (3) and in 1898 Martinus Willem Beijerinck (4) indicated the existence of an infective agent non-filterable and indemonstrable with the methods at their disposal. The advent of the electronic microscope in 1931 confirmed their theory and virology became a science.
This science has been confronted with the coronavirus, a respiratory virus already known for more than half a century (5) and already then studied in detail, which has generated a pandemic to include in a long list of epidemics and pandemics in recent times. The approach to this event however has been immediately discussed in the virological world in a very contrasting way, unusual for an established science (1+1=2 and not 3 or 4).
The various European governments, alarmed by the course of the epidemic, have more or less adopted the same transmission preventive measures such as: protective devices (masks and gloves), restrictions on movement, distancing even in the open, identification and isolation of healthy carriers.
ANALYSIS OF THE PREDISPOSING DEMOGRAPHIC AND GEOGRAPHICAL FACTORS
Before analyzing the efficacy of these protective measures on the epidemic, we need to consider other fundamental predisposing factors which affect the progress of the curves (Italy is considered to be representative for most European countries) for the following aspects:
1) Italian demographic aspect
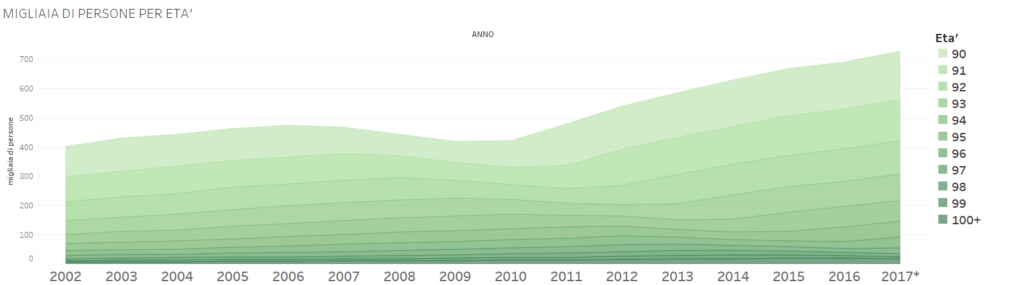
Since 2010 the number of over 90s has risen from about 400 thousand to about 700 thousand in 2017.
In 2018 those recorded aged over 85 were 2.2 million (highest figure in Europe according to ISTAT). This means a continuous increase in the number of elderly people in care homes. At present there are more than 300 thousand elderly residents in facilities in Italy. A number which corresponds to the city of Venice with its 260 thousand inhabitants, its 60 thousand odd tourists and its gondoliers included.

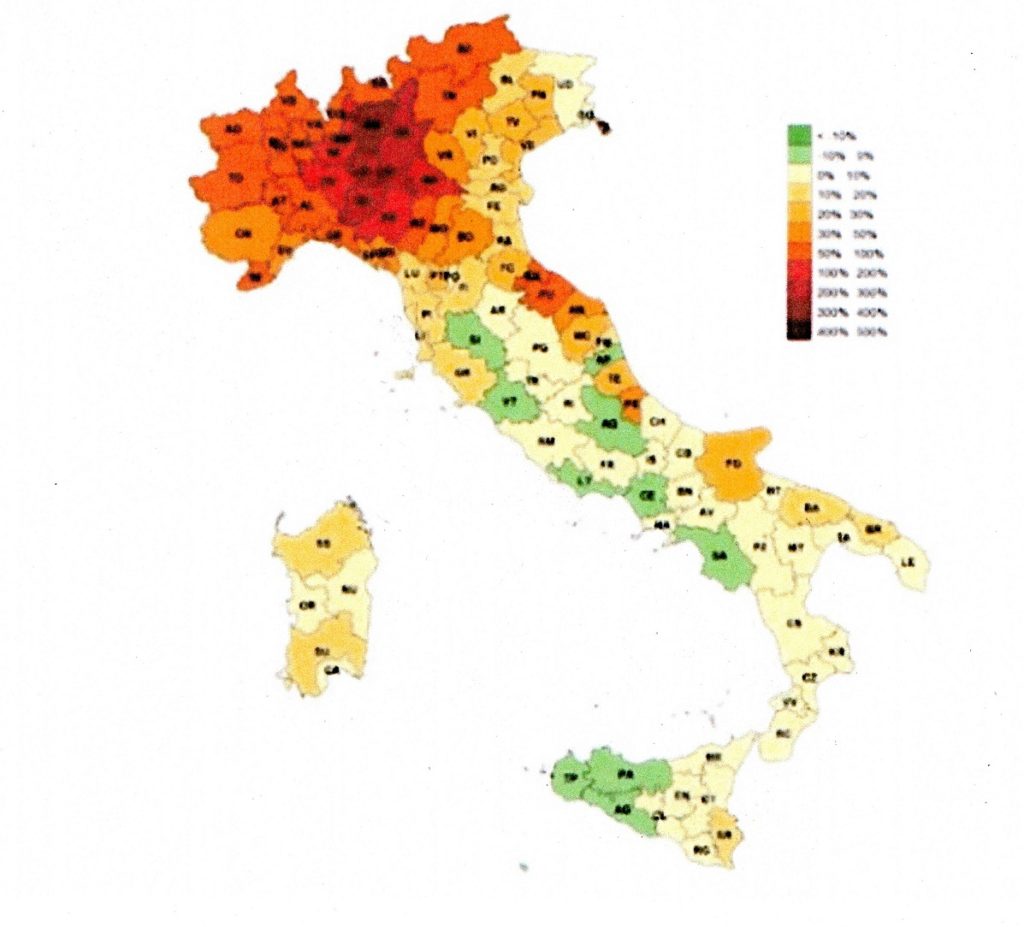
91% of the excess mortality occurred in the North with an increase of 52%, in the rest of the country it goes from an average increase in mortality of 1.1% down to an actual 5% reduction in mortality in Sicily. The more industrialized Northern areas were hit, with their specific environmental, climatic and working factors.
ANALYSIS OF THE PREVENTIVE MEASURES
A significant role of masks in relation to the transmission of viral infectious diseases has never been proved scientifically (7). Furthermore the advice/obligation to wear them does not take into account the regulations in force regarding their use (being work equipment(8)) as regards the time of use and their use by people with cardio-respiratory pathologies, pregnants and children. The lack of information on the risks incurred by their use, implies a serious risk to public health with even irreversible long term damage (9). But the use of masks is advised throughout the world, may be only to reassure the public.
Neither does distancing to reduce transmission of the virus in the population find any evidence in the medical literature regarding a possible reduction in mortality related to flu-like respiratory diseases and similar. Nevertheless, this measure is still in force in virtually any living environment both in the open (even on the beach, at the sea, at the stadium, public patron saints’ festivals etc.), and in indoor environments.
ANALYSIS OF THE EFFICACY OF THE MEASURES
In fact, there have been no significant variations in the course of mortality after the implementation of these measures. The mortality curve of the Influenza virus in 2016/17 and that of the Coronavirus, in 2019/2020(both respiratory viruses, similar to each other) have a statistically overlapping pattern.
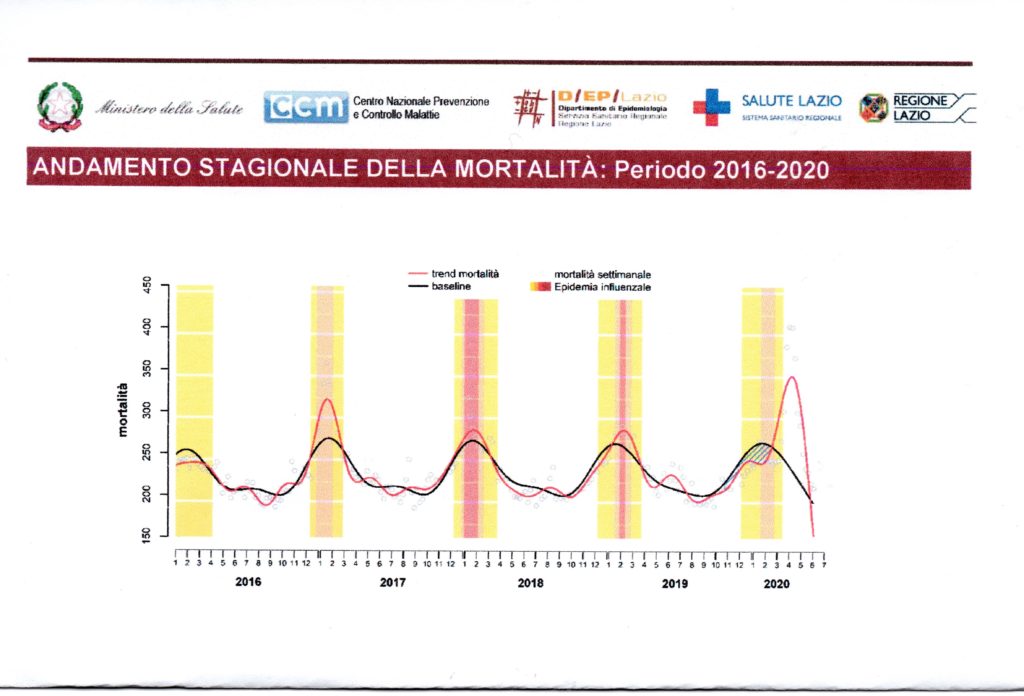
www.salute.gov.it/portale/covid/SISMG_sintesi.pdf del 15/06/2020 (10).
These represent two Gauss curves with identical slope parameters except for the height of the curves. Detracting the reduced mortality in the 4 months preceding the Coronavirus epidemic from the peak of the curve, there are no significant differences.
The reason for the failure of the measures undertaken, responsible for the constant increase in deaths, is determined by the insistence on the mistaken mode of transmission, (see title), previously considered through droplets or contact. The mode of transmission of the coronavirus is instead exclusively through aerosols, as already stated on 21/4/2020 to the scientific community (General observations on the Coronavirus (11), Aerosol as the only significant mode of transmission of Coronavirus (12)) and then also to various government and non-government bodies, finally in part accepted by the World Health Organization.
The behavior in the aerosols is comparable to passive smoking , whose particles, as regards dimensions, are superimposable (13).
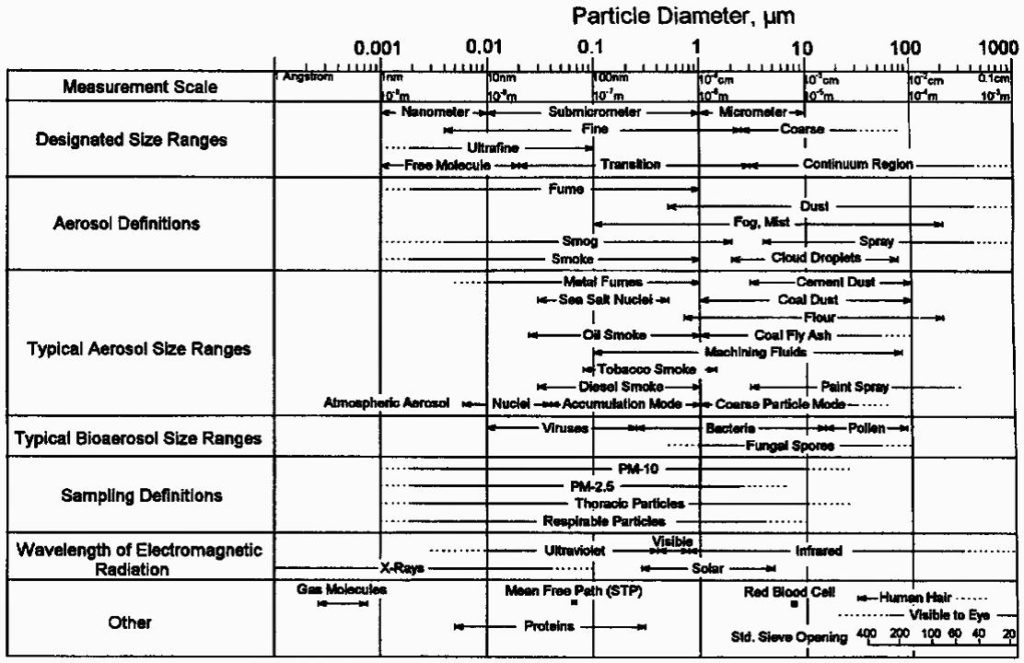

This evidence is further reinforced by observations in Germany, where many people in indoor environments have been infected (choir group, more than 1500 workers in a slaughterhouse). The high viral load, present in the form of aerosols, was due to the presence of asymptomatic people in the infectious phase and to the coexistence of other factors, including the conspicuous emission of the virus through increased respiratory activity (choir), the greater presence of the virus in the environment due to the low working temperature (slaughterhouse) and insufficient ventilation to reduce the sound dispersion (choir) and energy leakage (slaughterhouse).
CONSIDERATIONS ON THE NATURAL REPLY TO CORONAVIRUS
The dangerous transmission for health occurs in closed spaces (care homes, workplaces, offices, underground, conference halls etc), where the high viral load caused by insufficient ventilation (14) often leads to a serious evolution, especially in those with preexisting pathologies. As extensively demonstrated, the air quality in such environments is closely related to the risk of contracting infectious respiratory diseases (15) and in this specific case coronavirus.
In open spaces, but also in well ventilated indoor environments, this transmission occurs only with a very low viral load, similar to an active vaccine, which induces an immunological response with no evident signs of illness.
Anthropologically in closed communities the outsider was excluded, considered dangerous, while inside the community anti-distancing measures were applied to guarantee a passage of infective agents transmitted by aerosols (virus) even in the open. In Northern Europe it was sufficient to get less than a meter close for this mode of transmission, i.e. a handshake distance. In warmer countries aerosols are more volatile in the air, so a more intimate approach is necessary (a kiss on the cheek). In the Polar zones, transmission at a distance being impossible, it was ensured exclusively by rubbing noses.

If humankind had applied the laws laid down at present by most governments, it would have long been extinct
Therefore the replication factor, which indicates how many people are infected by an infected person, must be high in the healthy population (obviously the elderly or those with concomitant pathologies are shielded, as has always happened), thus guaranteeing the immunological memory essential for the survival of the species.
The identification of positives with apps like immune or through mass testing (at considerable cost to the community) and their isolation, seriously intervenes on the natural course of human defense against infectious diseases. Thus artificially creating the need for a vaccine again at considerable extra cost to the community.
There is a danger that the increase in mortality at the end of the summer, which happens every year like the winter peak during the flu epidemics, will be attributed to the Coronavirus (as already announced for months) and confirm the immediate national need for the vaccine.
CONSIDERATIONS ON VACCINATION
At present vaccine trials around the world, according to the WHO, are over 140 with multiple testing on people, all fast-tracked because of the emergency, with inherent dangers for the volunteers but also for the people employed in the research (see the terrifying experience in 1967 for the Marburg virus (16)). Moreover in phase 2 child volunteers are planned, in stark contrast to EU directives (17), which state “this objective can only be achieved through in-depth trials on drugs which may have significant clinical value for children”. This clinical value for children does not exist, because they are not affected by coronavirus, as demonstrated by most of the literature (18).
Considering the risks inherent in the trials, maybe it would have been wiser to limit these trials to a few centers around the world, authorized by ethics committees, which are, as postulated by the European Patients’ Academy (19): independent of sponsors, financiers, experimenters and undue influence (e.g. politicial, istitutional, professional or commercial).
The vaccine eventually obtained from these multiple trials, which do not respect the time normally considered necessary to guarantee a safe vaccine, puts those to be subjected to vaccination at serious risk, with at present unquantifiable but potentially very serious harm. Any doctor must remember the Hippocratic oath and must at least oppose the vaccination requirement for children, for whom there is no benefit from this treatment, only high risks.
CONCLUSIONS
With no intervention on the only mode of transmission of the virus (aerosols), populations continue to be exposed to a serious health risk. The precautions to be taken are neither masks (harmful) nor distancing (counterproductive), but adequate ventilation in buildings.
If these necessary preventive measures are not taken, a subsequent pandemic caused by another virus will alarm the political world again with all the consequences already experienced this year.
The history of medicine is steeped in great figures, who never feared contact with the sick, like Mother Teresa of Calcutta, Pasteur, Koch, Virchow, and great protagonists of the history of virology. Let’s not destroy their memory and their commitment, establishing medicine on false assumptions, which in the end will affect the weakest, our children (20).
BIBLIOGRAPHY
- https://www.google.com/search?q=codex+eschunna&oq=codex+eschunna&aqs=chrome..69i57j0l2.8426j0j4&sourceid=chrome&ie=UTF-8
- https://www.cambridge.org/core/journals/classical-review/article/celsus-de-medicina-aulus-cornelius-celsus-ueber-die-artzneiwissenschaft-ubersetzt-und-erklart-von-eduard-scheller-zweite-auflage-von-walther-frieboes-braunschweig-vieweg-und-sohn-1906-8vo-pp-xlii-862-tafeln-iv-m-18/083432E6C5C31FB9539507FA69583E42
- https://www.buecher.de/shop/fachbuecher/adolf-mayer-agronom/broschiertes-buch/products_products/detail/prod_id/31684669/
- https://www.britannica.com/biography/Martinus-W-Beijerinck
- https://www.vasodipandora.net/2020/05/30/virus-da-poco-conosciuto-e-ben-conosciuto-decenni/
- https://www.udinetoday.it/attualita/indagine-inps-decessi-coronavirus-maggio-2020.html
- https://www.ecdc.europa.eu/en/publications-data/using-face-masks-community-reducing-covid-19-transmission
- https://publikationen.dguv.de/regelwerk/dguv-regeln/1011/benutzung-von-atemschutzgeraeten
- https://www.vasodipandora.net/2020/05/29/coronavirus-and-masks/
- www.salute.gov.it/portale/covid/SISMG_sintesi_ULTIMO.pdf del 15/6/2020
- https://www.vasodipandora.net/2020/05/29/der-weltbildzertruemmerer-wegener-und-das-coronavirus/
- https://www.vasodipandora.net/2020/05/29/aerosol-als-der-einzig-relevanter-uebertragungsweg-des-coronavirus-epidemiologische-analyse/
- https://link.springer.com/chapter/10.1007/978-3-642-29942-1_16
- https://www.vasodipandora.net/2020/07/26/luft-ist-leben/
- https://pubmed.ncbi.nlm.nih.gov/12950586/ Rudnick and Milton
- https://www.tagesspiegel.de/gesellschaft/erster-ausbruch-des-marburg-virus-was-vor-50-jahren-in-den-behringwerken-geschah/20176074.html
- https://www.vasodipandora.net/2020/05/29/modell-zur-erklaerung-der-geringen-infektionsrate-bei-kindern-durch-das-coronavirus-epidemiologische-anatomische-und-physiologische-analyse/
- https://eur-lex.europa.eu/legal-content/IT/LSU/?uri=CELEX:32001L0020
- https://www.google.com/search?q=Comitato+etico+(CE)+-+EUPATI&oq=Comitato+etico+(CE)+-+EUPATI&aqs=chrome..69i57j33l3.6976j0j4&sourceid=chrome&ie=UTF-8
- https://www.vasodipandora.net/2020/07/26/children-and-coronavirus/
Correlated articles
General observations on the Coronavirus
The aerolsol as the only significant mode of transmission of the coronavirus: epidemiological evidence
Model to explain the low incidence of the coronavirus infection in children: epidemiological, anatomical and physiological analysis
Protective effect of smoking against Coronavirus
Coronavirus and masks
Air is live
Children and Coronavirus



